
The goal for many people with lower-limb amputations is to ambulate confidently with their prostheses and to return to a high level of social integration. To gain mobility, strength, and endurance, which contributes to increased physical activity and mental health, they need access to an active training program and monitoring by their multidisciplinary team.
Functions that are efficiently achieved by adults without amputations, such as climbing a ramp or walking with crutches, can become a significant hurdle for individuals with lower-limb amputations. In some ways, it’s more important for people with amputations to meet their physical fitness needs than those in the general community because a minor decrease in strength and endurance may diminish physical independence.1 The ability to walk is a strong determinant of health-related quality of life, allowing amputees to move around their environment more independently and safely, impacting their choice of activities and participation in them.
The rehabilitation process for people with lower-limb amputations is a complex task that ideally includes input from a multidisciplinary rehabilitation team. However, most often, physical rehabilitation and improving the walking capacity of these patients is the sole responsibility of physiotherapists. In this case, a physiotherapist should make sure to include some determinant actions in patients’ care: education for ongoing management of their prostheses, strategies for coping their limbs, and an active training program for resuming functional activities and enhance better living. The latter should include range-of-motion and mobility-enhancing exercises, balance, and strength training in combination with aerobic training, all of which promote walking capacity.2
Structured Exercise
Given the cost of healthcare provision and the anticipated growth in demand for rehabilitation, delivering adequate care is challenging, and a structured home exercise training program can help.3 Exercise training is a valid therapeutic method to improve muscle strength and endurance, locomotor performance, and to decrease cardiovascular risk factors.4 However, no evidence-based best practice guideline for physiotherapy for people with lower-limb amputations has been established. In general, studies show the importance of strengthening exercises as well as gait training for prosthesis use.5,6
Exercising contributes to the general physical and psychological well-being of patients and can be initiated at any moment in patients’ rehabilitation, considering the minimal conditions for regular mobility are met. Their circulation problems, prosthesis control, walking, balance, postural stability, and energy consumption can all be improved.6
It is crucial to ensure that lower-limb prosthesis users know which types of exercises and platforms they can use to improve their rehabilitation and continuity of care, but it is also imperative that the exercises are built up gradually to reduce the risk of skin abrasion and consequent delay in the fitting process.4
Regaining functional independence requires the repetition of some exercises to the point of annoyance, causing some loss of motivation. The integration of virtual reality, video games, and tactile interface apps into conventional physical rehabilitation may contribute to motivation and promote adherence to prosthetic use and training programs as they provide an interactive and engaging form of exercise.
Gamification of rehabilitation is a concept that is being increasingly introduced in the profession and using game design elements in the therapeutic context has proven to increase its effectiveness across many healthcare areas.7 The introduction of serious games in the rehabilitation process makes it more fun and motivating, but it is not short of complexity, clinical value, and adaptability to specific patients and conditions. Often, a therapist can adapt a certain game’s difficulty (targeted for a specific rehabilitation process) according to a patient’s evolution, for example by penalizing compensatory movements. Also, a major advantage of digitizing care is the collection of meaningful data, which can be saved in every session and analyzed for a better comprehension of patients’ conditions and evolution. More importantly, with the help of gamification, the users will feel like players and not like patients, while engaging and getting a more profound understanding of their self-care.
Monitoring Progress
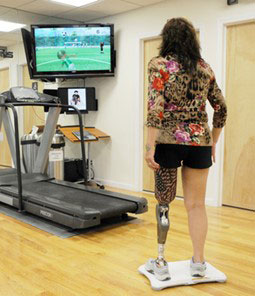
Virtual reality can be used by lower-limb prosthesis users when simulating real activities in a safe environment.8 The practice intensity can be manipulated, and therefore individualized treatments can be provided by the rehabilitation team. Virtual reality provides information about motor movements (performance) and outcomes of those movements (result) that can be used to monitor patients’ evolution.9
Several games for rehabilitation gamification are adaptations of familiar off-the-shelf solutions. Video game accessories such as Nintendo Wii Fit and Xbox Kinect are examples of these technologies. Imam et al. the prevalence of using commercial games in lower-limb prosthetic rehabilitation and which types of games were being used by therapists across Canada.10 The study showed that half of the respondents used commercial games in their lower-limb prosthetic practice, mostly Nintendo Wii Fit. Numerous other studies have reported similar results.11,12 Over 70 percent of the participants with disabilities enjoyed the Wii Fit intervention more than their usual therapy and about 90 percent expressed that they would like the program to be added to their usual therapy.13
Users interact with Wii Fit games through weight-shifting while standing on the balance board or while using a handheld remote control. The balance board’s sensors measure the users’ center of pressure and weight distribution. The Wii Fit exercises/games can stimulate static and dynamic balance and stationary gait training, all of which are critical to improve prosthetic walking. Wii Fit includes a yoga game, mainly targeted to static balance training (maintenance and transition between static poses), along with dynamic balance games (involving the simulation of sliding and different body tilts), strength training (adding complexity and rewarding endurance on typical gym routines), and aerobic exercises (which have extra rhythm and speed), focused on dynamic balance and gait training.9
Another video game accessory used by some physiotherapists is the Xbox Kinect. Xbox Kinect may hold greater promise for use in rehabilitation because of the advanced motion tracking technology that it uses; however, compared to the Wii Fit, it is less commonly used in rehabilitation and the research evidence for its use in rehabilitation is still limited.10 Moreover, despite being a promising platform, Xbox Kinect’s production was discontinued in 2017.
Rehabilitation games are also being developed for tactile interfaces, such as regular tablets. Ottobock launched Fitness App, which includes different exercises for people with upper- and lower-limb amputations. For people with lower-limb amputations, the training is divided into three modules that can have different levels of difficulty: Strength and Endurance, Coordination and Balance, and Stretch and Relax. The first module demonstrates classic exercises for strength and endurance training without the prosthesis. The second module focuses on balance and coordination training with the prosthesis, targeted to improve patients’ control while performing activities of daily life. The third module helps muscular relaxation and promotes faster recovery after training.14
Individuals with lower-limb amputations have unique needs and require specialized management expertise to facilitate optimal outcomes and recovery. They can live in remote areas, have limited or no access to existing rehabilitation programs, and even be further limited by restrictions, such as the lockdowns imposed during COVID-19, where these types of training are fundamental to keep them active and motivated during their rehabilitation process. Also, some of these training options can be integrated with telehealth, allowing continued monitoring of evolution and providing the ability to connect amputation care experts with patients in more remote or underserved areas where services are not available.15

In conclusion, it has become obvious that the application of a home treatment intervention and training in people with lower-limb amputations can benefit beyond improved walking capacity and include improvements in physical activity tolerance, adaptation to activities of daily living, and participation in the community, which may ultimately lighten social and financial costs.16
Acknowledgement: The author wishes to thank Marina Castro, MBE, and Ana Sofia Assis, MBE, biomedical engineers at Adapttech, for their critical input.
Vanessa Carvalho, CPO, is a clinical specialist at Adapttech, adapttech.eu. She has been in O&P since 2015 and joined Adapttech in December 2021.
References
- Bin Yar, U. 2021. Activities for physically disabled in isolation of COVID-19 pandemic. Journal of University Medical & Dental College 12(3). doi:10.37723/jumdc.v12i3.544.
- Esquenazi, A., R. DiGiacomo. 2001. Rehabilitation after amputation. Journal of the American Podiatric Medical Association 91(1):13-22. doi:10.7547/87507315-91-1-13.
- Lusardi, M., C. Nielsen. 2007. Orthotics and prosthetics in rehabilitation. Saunders Elsevier.
- International Committee of the Red Cross. 2020. Exercises for Lower-Limb Amputees. www.icrc.org.
- Almeida, L., C. Fukuchi, T. Sakanaka, A. Cliquet. 2021. A low-cost easily implementable physiotherapy intervention clinically improves gait implying better adaptation to lower limb prosthesis: a randomized clinical trial. Scientific Reports 11(1). doi:10.1038/s41598-021-00686-9.
- Ülger, Ö., T. Yıldırım Şahan, S. Çelik. 2018. A systematic literature review of physiotherapy and rehabilitation approaches to lower-limb amputation. Physiotherapy Theory and Practice 34(11):821-834. doi:10.1080/09593985.2018.1425938.
- Steiner, B., L. Elgert, B. Saalfeld, K. Wolf. 2020. Gamification in Rehabilitation of Patients With Musculoskeletal Diseases of the Shoulder: Scoping Review. JMIR Serious Games 2020 8(3):e19914 https://games.jmir.org/2020/3/e19914. doi:10.2196/19914.
- Abbas, R., D. Cooreman, H. al Sultan, M. el Nayal, I. M. Saab, A. el Khatib. 2021. The Effect of Adding Virtual Reality Training on Traditional Exercise Program on Balance and Gait in Unilateral, Traumatic Lower Limb Amputee. Games for Health Journal 10(1):50-56. doi:10.1089/g4h.2020.0028.
- Imam, B., W. Miller, L. McLaren, P. Chapman, H. Finlayson. 2013. Feasibility of the Nintendo WiiFitTM for improving walking in individuals with a lower limb amputation. SAGE Open Medicine. 1:205031211349794. doi:10.1177/2050312113497942.
- Imam, B., W. Miller, H. Finlayson, J. Eng, T. Jarus. 2018. A clinical survey about commercial games in lower limb prosthetic rehabilitation. Prosthetics and Orthotics International 42(3):311-317. doi:10.1177/0309364617740238
- Forsberg, A., Nilsaga˚rd Y, Boström K. 2015. Perceptions of using videogames in rehabilitation: a dual perspective of people with multiple sclerosis and physiotherapists. Disability and Rehabilitation 37(4):338. doi:10.3109/09638288.2014.918196
- Goble, D., B. Cone, B. Fling. 2014. Using the Wii Fit as a tool for balance assessment and neurorehabilitation: the first half decade of “Wii-search.” Journal of NeuroEngineering and Rehabilitation 11(1):12. doi:10.1186/1743-0003-11-12
- Meldrum, D., A. Glennon, S. Herdman, D. Murray, R. McConn-Walsh. 2012. Virtual reality rehabilitation of balance: assessment of the usability of the Nintendo Wii® Fit Plus. Disability and Rehabilitation: Assistive Technology 7(3):205-210. http://dx.doi.org/103109/174831072011616922. doi:10.3109/17483107.2011.616922.
- Fitness for Amputees app | Ottobock SE & Co. KGaA. www.ottobock.com/en/apps/fitness-app
- Webster, J., P. Young, J. Kiecker. 2021. Telerehabilitation for Amputee Care. Physical Medicine and Rehabilitation Clinics of North America 32(2):253-262. doi:10.1016/j.pmr.2020.12.002.
- Imam, B., W. Miller, H. Finlayson, et al. 2014. A Telehealth Intervention Using Nintendo Wii Fit Balance Boards and iPads to Improve Walking in Older Adults With Lower Limb Amputation (Wii.n.Walk): Study Protocol for a Randomized Controlled Trial. JMIR Research Protocols 3(4):e80. doi:10.2196/RESPROT.4031.





