
Children with low tone need early orthotic intervention to prevent gait problems down the road.
When Ting Cusick arrived in the United States in 1998, the newly adopted one-year-old had nonfunctioning lax hips and feet. But despite these early setbacks, Ting began walking at 14 months, four months earlier than the average Chinese infant, according to her mother, Beverly Cusick, MS, PT, BOC COF.
Ting is now 13 years old and excels in soccer, skiing, gymnastics, and cheerleading. Her mother, a pediatric physical therapist, attributes some of her daughter’s athletic success to wearing heel seats in canvas shoes with laces, flat soles, and deep heel boxes, beginning when she was 12 months old.
Although many pediatricians and orthopedic surgeons won’t recommend foot orthotics for pronated feet in patients younger than five—saying that children undergo significant developmental changes during their first five years—many orthotists and physical therapists, such as Cusick, argue that it’s important to intervene much earlier. These practitioners recommend intervening anywhere from 18 months to two years of age; however, some recommend orthotic intervention as early as when a child begins to stand, and for some infants born prematurely intervention can occur before the child’s due date.
“The physician’s ‘party line’ on pronated feet seems to be, ‘Don’t worry, she’ll outgrow it,'” Cusick says, adding that only pronation occurring in a “sound pediatric foot” corrects without intervention. According to Cusick, “children with feet that will not improve over time are dismissed, and they will load their pronated feet two-million times per foot per year in pathomechanical alignment that communicates up the leg to the torso.” Muscle fatigue while walking and increasingly stiff leg muscles are common complaints in children, adolescents, and adults who have retained persistent foot pronation, she says.
Challenging Conventional Wisdom

“When infants show excessive foot pronation at the time they begin to pull to stand and cruise—around age seven to nine months—the fragile ligaments and underdeveloped foot muscles are at risk for enduring deforming strains that will not recover spontaneously,” Cusick says. “The goal is to capture and tip the excessively tilted heel back into a more appropriate alignment for taking body weight while leaving the forefoot active and operative.”
Debbie Strobach, PT, MA, is a pediatric splinting specialist at St. John’s Mercy Medical Center, St. Louis, Missouri, and has been creating AFO-type splints using low-temperature thermoplastic for low-tone infants in the neonatal intensive care unit (NICU) for 20 years. She puts splints on infants with low muscle tone before they start standing—anywhere from birth to 12 months—including infants with trisomy 21, congenital myopathy, benign hypotonia, prematurity with muscle imbalance, and other conditions. Strobach says early splinting allows her to minimize the ankle-foot deformity before babies begin to pull to standing independently or begin standing in therapy with assistance. Once the child can stand, Strobach will use an AFO, SMO, or UCBL that is appropriate for the child’s alignment to prevent and/or correct the deformity.
“When you first see the deformity, why wait and let the deformity get worse?” she asks. “If you have an infant that you know has low muscle tone, those children are probably not going to improve their alignment without help.”
 |

|
| Left: Ting competes in a regional gymnastics event. Her balance is no longer affected by her low tone. Right: Ting “has always been a fearless and aggressive soccer player,” says her mother, Beverly Cusick, PT. |
Premature infants may have a developmental imbalance in the strength of the peroneus longus and peroneus brevis muscles, Strobach says. This imbalance overpowers the anterior and posterior tibialis, which translates to ankle eversion posturing and later pronation deformities once the child begins standing. Without taping and splinting interventions in the NICU, these infants may show excessive calcaneal valgus in their initial standing posture as they reach the end of their first year. If, on the other hand, the hypotonic baby is splinted in the NICU, the child will most likely require splints for several months, Strobach says. If splinting commences when standing is initiated, the child will usually need splints until age two or three, with the splints being discontinued when the child begins to show age-appropriate alignment and gait, Strobach notes. Without early splinting or foot orthotics, these children may require orthotic intervention to correct their alignment until they are seven- or eight-years old.
“If we can get them early during the first year, we can usually totally correct this before they are standing,” Strobach asserts, adding that the goal is to minimize the deformity before the child starts walking.
By age four, Ting had progressed to wearing prefabricated plantar-level insoles to optimize her functioning foot-joint alignment and weight-load distribution, as well as her developing knee and hip-joint alignment. Ting continues to wear the plantar shoe inserts, as “her Asian heritage dictates that her foot joints are more lax than those of Caucasians,” Cusick says.
When to Intervene
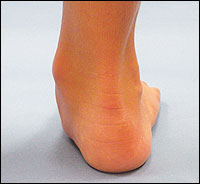
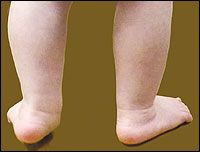
Children with low muscle tone can develop lax ligaments, which inhibit joint stability in the foot and ankle complex. In hypotonic patients, the heel tilts into valgus, and the weight line shifts medially, causing the midfoot to collapse. Once the feet are pronated, the knees and hips also become misaligned. This means the muscles that move those joints no longer work efficiently, and it takes more energy for these children to do the same work as their non-pronated peers.

Orthotists typically do not intervene before a child starts to pull to standing, but many say they begin orthotic intervention soon after, especially if a child is diagnosed with a developmental disability, such as Down syndrome, where it’s known that the child’s low-tone condition will be lifelong.
“These are the children you want to brace early, right as they show signs of pulling to stand,” says Curt Bertram, CO, who works at the Hanger Prosthetics & Orthotics patient care facility in Hartland, Wisconsin. He adds that children with low tone have ligamentous laxity, which causes hypermobility of the joints and results in pronation of the feet and ankles, which will worsen as the child progresses into adulthood. Bracing early will help these children’s bones grow normally, he adds.
“We need to work with our pediatricians to show them that early orthotic intervention with children diagnosed with Down syndrome is needed to prevent abnormal growth due to poor position from ligamentous laxity and hypermobility,” Bertram urges. “These low-tone kids fall into pronation, so it’s our job as orthotists to hold them in good biomechanical alignment. Don’t play the waiting game with these patients. We don’t want to create permanent deformities.”
Kevin Matthews, CO, LO, owner of Advanced Orthopedic Designs, San Antonio, Texas, agrees. “I have seen many incidences where bracing was definitely indicated, but the pediatrician said these deviations were within normal limits,” he says.
Even if the pronation might have self-corrected over time, it’s better to err on caution’s side and intervene early, Matthews advises, adding that he’s more aggressive than some orthotists. He typically recommends orthotic intervention if the patient’s talocalcaneal valgus angle is five degrees or greater. His patients are as young as 18 months old.

Bernie Veldman, CO, owner of SureStep and Midwest Orthotic Services, South Bend, Indiana, agrees that the degree of heel valgus is the best determinant for early intervention. The heels of most children with low tone will fall into the 10-to-20-degree range, he says.
“If the orthoses are made correctly, I feel there are no significant negatives associated with early intervention,” Matthews says, but he cautions that waiting can result in significant foot deformities. “Hypotonic kids left unbraced will invariably end up with equinus contractures, requiring surgery to bring the foot-ankle complex into normal alignment,” he explains.
Matthews has seen eight-year-old hypotonic children with Down syndrome who have “terrible bunions,” because they never wore corrective orthoses. Children with hypotonia have true triplanar instability, he explains, where the tibia internally rotates on the talus, the talus will externally rotate, the heel slides off into valgus, and the midfoot collapses into pronation or flat-footedness and the forefoot slides into abduction which leads to bunions, where the big toe deviates medially toward second toe.
“I believe that of the kids who have five degrees or less of valgus at the heel, 50 to 80 percent will outgrow it without intervention, but we don’t know which ones will and which ones won’t,” Matthews says. “So why not brace? All we are doing is giving the child structural support. We are not taking away from the musculature. We are not making the muscles weak. Why wait until age five because by five the malalignment may well be more severe, especially for those who have accompanying diagnoses like Down syndrome.”
For a child who has low tone and flat feet but doesn’t have heel involvement, Matthews usually recommends foot orthotics such as pre-made shoe inserts.

“Any time I can provide a child with a better static stance or a noticeably higher level of functional ambulation, I see this as an opportunity that shouldn’t be passed by,” says Ethan Leavitt, CPO, from Mary Free Bed Rehabilitation Hospital, Grand Rapids, Michigan, who notes that he once casted a six-week-old premature baby a week before the baby’s due date. “It’s not a matter of age. It’s a matter of whether or not I can improve their posture in weight bearing, their pattern of ambulation, and even their quality of life in a small way. I have seen many, many kids stand up and walk so much better—even run for the first time—after being fit with lower-extremity orthoses.”
Leavitt says that whether a child needs an orthosis depends on whether there are joint deformities and whether the patient’s condition has worsened over time. For children who are walking, he also looks at the quality of the child’s gait and if there is a varus or valgus deformity.

When deciding whether or not to intervene, Don Buethorn, CPO, owner of Cascade Dafo, Ferndale, Washington, looks at whether developmental concerns are present, and if so, he typically recommends bracing as soon as the child begins standing.
“When the foot is visibly pronated, when…they are [assessed as being] behind in their motor skills, then I advise using appropriate orthotic intervention,” Buethorn notes. “I believe the daily practice of enhanced balance and movement in conjunction with a richer sensory experience supports the best development of the patient’s motor-skill potential.”
For children with mild low-tone pronation without a neurological deficit, Buethorn recommends a shoe insert. “Research shows that shoe inserts work,” he says.
The Goal Is in the Gait
Children with low tone tend to walk late because their feet and ankles are in poor alignment and their toes often claw at the ground for stability, causing their feet to tire, Veldman says. Pronation resulting from lax ligaments in children with low tone usually cannot be improved, but what can be improved is the way children learn to walk, he notes.
“Children learn all gross motor skills in the first seven or eight years of life,” he maintains. “That is the ingrained gait pattern. If we can get these kids at 12 months, or when they show an interest in standing, and stabilize their feet while they are developing these skills, then they have the opportunity to develop these skills properly.”
The idea, Veldman explains, is to create stability, initially by stabilizing the heel in a midline position. He says flexible, dynamic SMOs “program” a child’s gait while improving alignment. With enough repetitions, the child will carry that gait pattern into adulthood. Gait quality determines how much energy is used with each step; those whose feet have not been stabilized will tire easily and likely become sedentary. These children often gain weight, and it becomes difficult to get them active again. Often, these children will also be less coordinated and fall frequently.
Matthews agrees that the goal of bracing is to improve the structural alignment of the muscles so that kids don’t tire as easily, and their balance, endurance, and coordination improve. Orthotic intervention includes maintaining the heel in vertical alignment, providing mild support for the arch, and using a long lateral or extended lateral trim to capture the fifth metatarsal head to prevent the forefoot abduction.
Problems with Bracing
Overbracing or underbracing can cause problems, according to Veldman. Overbracing with rigid plastics tends to immobilize the foot so the foot can’t function normally, he says. “If you put the foot against a hard piece of plastic and take away its movement, it will cease to function, and the muscles will atrophy,” he adds. “In order to stabilize the foot and allow it to behave normally, [the brace] needs to be [made from] a plastic that’s firm enough to stabilize the foot in a normal position and flexible enough to allow the foot to move naturally through the gait cycle.”

For example, John Izak, CPO, co-owner of Philadelphia, Pennsylvania-based Orthologix, says he prefers flexible SMOs over the more rigid designs that have been traditionally used to manage the hypotonic foot. The devices are manufactured with thin plastic and specific trim lines that terminate medially behind the first metatarsal and laterally to the toe sulcus. These trimlines, coupled with a neutral heel and compression created by the plastic, stabilizes the foot. This in turn normalizes the distribution of forces from rearfoot to forefoot in weight bearing.
“If we as orthotists balance these feet and manage them correctly, we are giving the knees and the hips a stable base,” Izak says. “These influences on maturing bones and joint alignment are critical for healthy skeletal alignment.”
Izak says that by using this type of orthosis, he has seen younger children attain their developmental milestones sooner, and older children run, jump, and play with their age-matched peers.
Underbracing with foot orthoses tends to create more problems than it helps, Veldman asserts, partially because calluses and sores can develop, and then children won’t want to wear them. “Underbracing with a foot orthotic doesn’t…do much good,” he says. “It’s trying to address the arch, and the arch isn’t the problem. It’s all about the heel.”
How Long?
Cusick says that children should wear foot-alignment assistive devices during all waking hours, as long as the devices were chosen appropriately and the child is comfortable and fully functional in them. She adds, however, that no one can predict the length of wear time needed to optimize bodyweight distribution through the feet. The number of repetitions of ideal weight shifts onto and loading through the feet—together with the physiologic adaptation of the bones, joints, muscles, connective tissues, and brain—determines the duration of wear.
Susan Glairon is a freelance writer who lives in Longmont, Colorado.





