Capstone Project Completed at Eastern Michigan University
In addition to O&P patient evaluation and device fabrication and fitting, certified O&P clinicians are responsible for patient education (PE) regarding those devices and services.1,2 In hospital settings, the quality of PE upon discharge is statistically negatively correlated with readmission rates. Readmission often represents preventable healthcare costs, and can leave patients feeling dissatisfied in their healthcare and unhappy with their ability to manage their own health.4 Yetzer states that healthcare professionals are responsible for patient education to provide information, assessing each patient’s understanding of the information, and restating the information as necessary for understanding.3
Literacy level, culture, language, and physiological barriers are obstacles found in nursing studies focused on PE.5 One study classified barriers to providing PE as they related to the patient, healthcare provider, and physical environment.6 Per the American Board for Certification Orthotics, Prosthetics & Pedorthics (ABC), O&P patient care accreditation and applicable Centers for Medicare & Medicaid Services guidelines, O&P practitioners are required to provide verbal and written instructions upon delivery of O&P devices to educate the patient about how devices operate, how to don/doff them, and their proper care and maintenance.7,8 Quality patient education may empower patients, increase their participation in the treatment plans, improve acceptance of their devices, and minimize noncompliance.9 While verbal and written information are useful, research has demonstrated that including additional PE materials is more effective in educating patients.10,11 No literature has been found regarding PE in O&P.
The goal of this project was to gain insight into O&P practitioners’ perspectives on PE, to identify potential barriers to PE, and collect information regarding the provision of PE in O&P.
Methods
A single, anonymous, online survey consisting of 11 demographic questions and 24 PE questions was conducted. The survey was a modified version of the Nurses’ Patient Education Questionnaire (Likert scale/open-ended).12 It was modified to include questions regarding barriers to PE, information on provision of PE, and O&P professionals’ perspectives on PE. The survey received internal review board approval and a consent form was placed at the start of the survey, which can be viewed at forms.gle/Ykt2UScYa3xujHvD8.
The survey was open to practicing professionals in O&P with designations of CPO, CO, CP, LPO, and/or CPed. Subject data was excluded if the respondent was a resident, retired, or held a different certification from the aforementioned.
Recruitment for the survey was done via two posts three weeks apart on LinkedIn and two emails three weeks apart on the OANDP-L listserv.
Descriptive statistics (means and proportions) and correlations were conducted. Google Sheets was used for means and proportions. Thematic analysis was conducted to categorize and track the answers to the open-ended questions. Technological self-efficacy (TSE) was scored using three questions about technology from the survey. A Chronbach’s alpha was used to see how related the three technology questions were. Pearson’s r correlations were done to see if there was correlation between age, TSE, and the percentage of time respondents said that they spent with patients in each appointment.
Results
A total of 119 respondents completed the survey. After exclusions, there were 113 respondents included in the results. There were 72 males, 40 females, and one preferred not to say. This ratio corresponds favorably with ABC practice analysis data (Figure 1). The average age of the respondents was 45.3 years old. Among the respondents there were 74 CPOs, 19 COs, 17 CPs, two LPOs, and one CPed. Thirty-eight percent of respondents reported that they obtained a master’s degree or higher. Approximately 85 percent of respondents reported learning about the importance of PE in their formal education.

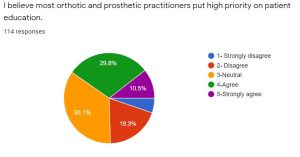
Fifty-seven percent of respondents said that they always have time for PE, while 33 percent reported they almost always have time for PE. Respondents listed that on a normal workday they devote approximately 21 percent of each patient appointment to PE. Using a Likert-scale question with a scale of one to five, when respondents were asked whether they believe other practitioners in the field put priority on PE the mode was three, but when asked if they put high priority on PE the mode was five. The complete full results of these questions are listed in Figure 2.

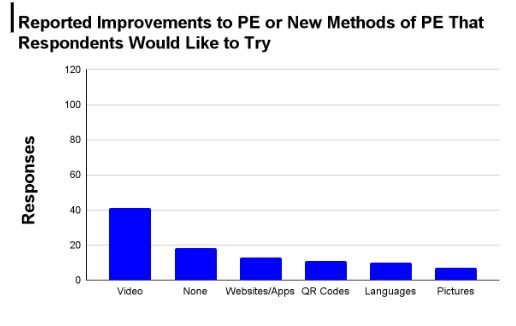
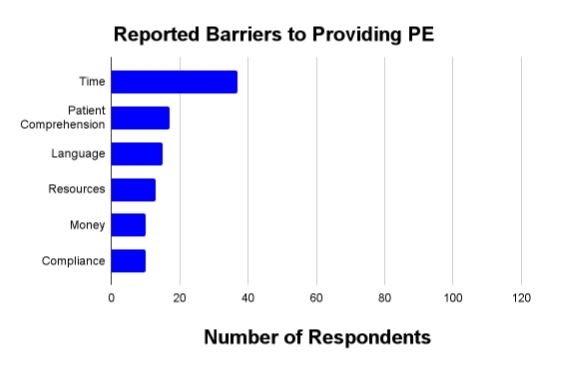
When asked the types of PE that they use most frequently with patients, 87 (77 percent) selected verbal PE and 79 (70 percent) selected written PE. Ten percent of respondents reported using videos, internet, QR codes, or demonstrations frequently. Thirty-four respondents (29 percent) reported language barrier as a reason why they have had to adapt their normal PE methods, 29 (24 percent) mentioned patient comprehension, and 25 (21 percent) mentioned visual/hearing impairments. Forty-three (36 percent) respondents mentioned that they would like to improve their video PE or begin to use it more (Figure 3). Time, patient comprehension, and language were the most frequently listed barriers to providing optimal PE (Figure 4).
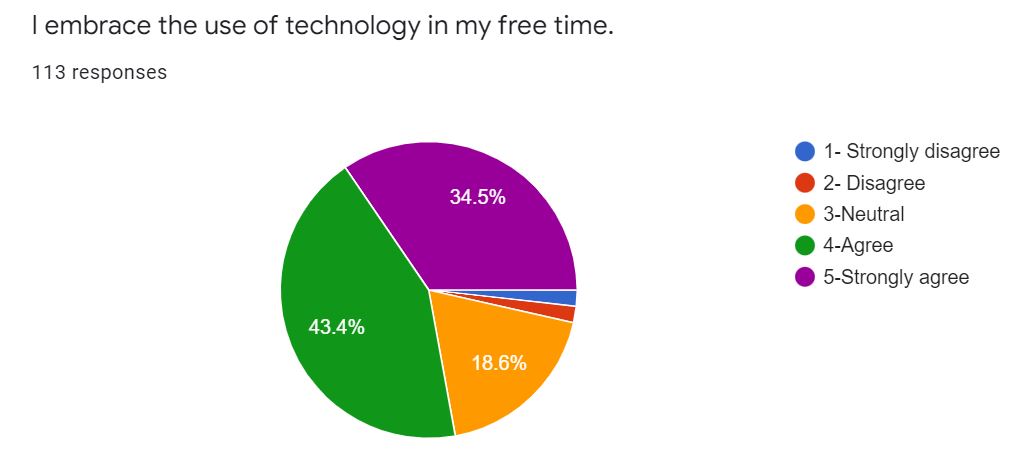
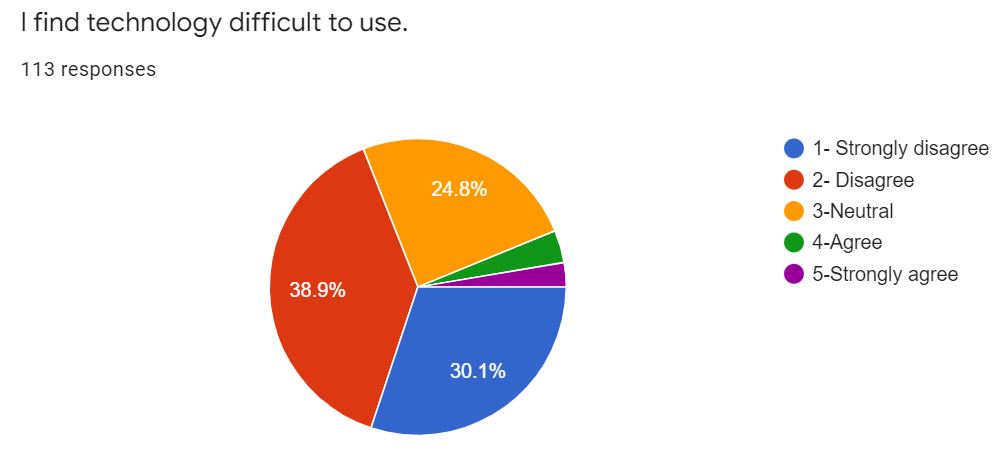
The results of questions regarding technology are listed in the charts in Figure 5. A Chronbach’s alpha was computed for the three questions with a value of .648 indicating good to very good on the relation of the three questions as a group.


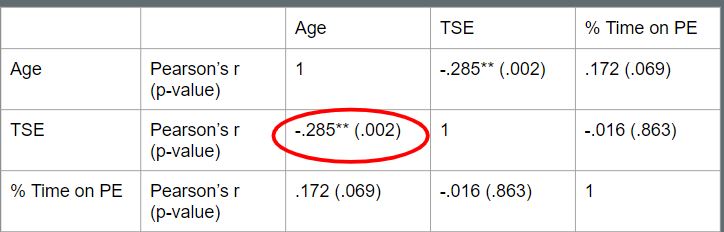
There was one statistically significant correlation found between age and TSE (Figure. 7). The correlation was -.285 with a p-value of .002.
Discussion
The results suggest that professionals in O&P believe that they personally put high priority on PE but are mostly neutral regarding how others in O&P put high priority on PE. In this survey, a negative correlation was found between age and TSE, which may indicate that the older the practitioner, the lower their belief that they can successfully complete tasks with technology.
The responses in this study also indicate that a high percentage of O&P professionals are using only written and verbal PE with their patients. This is the minimum requirement, but based on the literature, patients may benefit from receiving more types of PE along with the written and verbal types. There were many respondents who reported having access to internet, videos, and QR codes, but few report using them frequently with their patients. This suggests that the barriers listed in this survey may be preventing O&P professionals from using them. Barriers listed to providing quality PE in this survey were similar to the literature on nursing PE barriers.
Some interesting comments from respondents regarding hurdles that they face included the idea that profit-first mindsets, reimbursement issues, poor quality PE resources, and clinician motivation often lead to poor PE quality in O&P. Multiple respondents stated that they wish there were more ways to easily individualize PE that patients could take home, or access from home. Some respondents of the survey suggested that a standardized PE resource could be developed for the profession by one of the major O&P organizations. Others stated that the profession needs to fight for reimbursement of our time so we can spend more time on PE.
A limitation of this study is that nearly 35.4 percent of the respondents were from Michigan (where the researchers’ institution is located) or Minnesota, although there were respondents from 30 states. The internal biases of the respondents who decided to do the survey could also be a limitation that affected the data.
Conclusion
Literature from O&P governing organizations and the perceptions of O&P professionals in this survey indicate that PE is an important and necessary component of O&P practice. The results of this survey suggest that more time should be allocated to provision of PE to patients, and attention should be placed on developing quality PE resources. Additionally, clinicians recognize the need for adapting PE to better align with patient needs with respect to comprehension and language barriers.
Future research in this area should include a larger sample size and an attempt to reach a broader audience geographically. A survey with more comprehensive questions to address TSE and barriers more thoroughly may prove useful. Gaining patient perspectives on PE types in O&P could also be valuable as a way to inform future PE option decisions.
Jace Briggs, MSOP, recently graduated with a Master of Science in Orthotics and Prosthetics from Eastern Michigan University. Briggs is performing a dual 18-month combined residency with Walkabout Orthotics and Prosthetics, Wausau, Wisconsin.
Acknowledgements:
Frank J. Fedel – Advisor
Sun Hae Jang – Tested survey and gave feedback
Samantha Eckert – Tested survey and gave feedback
Tara Wright – Tested survey and gave feedback
References:
- opcareers.org. What is O&P? 2021
- Ncope.org. 2021
- Yetzer, Elizabeth A. MA, MSN, CRRN Education of the Patient With Neuropathic Limb, JPO Journal of Prosthetics and Orthotics: April 2005 – Volume 17 – Issue 2 – p S45-S49
- Luther B, Wilson RD, Kranz C, Krahulec M. Discharge Processes: What Evidence Tells Us Is Most Effective. Orthop Nurs. 2019 Sep/Oct;38(5):328-333.
- Beagley L. Educating patients: understanding barriers, learning styles, and teaching techniques. J Perianesth Nurs. 2011 Oct;26(5):331-7.
- abcop.org. Patient Care and Management (PC). 2021.
- Center for Medicare Advocacy. Delivery and Set-Up Guidelines for Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS). July 10, 2014
- Melton, Danielle H. MD Physiatrist Perspective on Upper-Limb Prosthetic Options: Using Practice Guidelines to Promote Patient Education in the Selection and the Prescription Process, Journal of Prosthetics and Orthotics: October 2017 – Volume 29 – Issue 4S – p P40-P44
- Boyde M, Tuckett A, Ty J. Teacher-as-actor: Investigating the barriers and facilitators of patient education among hospitalized patients in a cardiology clinical unit. Nurs Health Sci. 2021 Dec;23(4):871-879.
- Friedman AJ, Cosby R, Boyko S, Hatton-Bauer J, Turnbull G. Effective teaching strategies and methods of delivery for patient education: a systematic review and practice guideline recommendations. J Cancer Educ. 2011 Mar;26(1):12-21.
- Wilkin ZL. Effects of Video Discharge Instructions on Patient Understanding: A Prospective, Randomized Trial. Adv Emerg Nurs J. 2020 Jan/Mar;42(1):71-78.
- Bergh A-L, Johansson I, Persson E, Karlsson J, Friberg F. Nurses’ Patient Education Questionnaire – development and validation process. Journal of Research in Nursing. 2015;20(3):181-200. doi:10.1177/1744987114531583




