 In 1981, The O&P Almanac published an article by John Sabolich, CPO, titled “Professionalism Or What?” in which he challenged practitioners to update their practices to reflect a more contemporary, patient-centered focus.1 “Sometimes the words that come out of our own mouths are the greatest obstacles to being fully recognized as professionals….We call our patients ‘customers,’ our lab and office a ‘shop’ or ‘store’; our fee schedules are called ‘price lists.'” Contrast this with the strong sentiments that a prosthetics student with a transtibial amputation expressed during a group discussion in one of my behavioral science courses: “Don’t call me ‘a patient’—I’m not sick.”
In 1981, The O&P Almanac published an article by John Sabolich, CPO, titled “Professionalism Or What?” in which he challenged practitioners to update their practices to reflect a more contemporary, patient-centered focus.1 “Sometimes the words that come out of our own mouths are the greatest obstacles to being fully recognized as professionals….We call our patients ‘customers,’ our lab and office a ‘shop’ or ‘store’; our fee schedules are called ‘price lists.'” Contrast this with the strong sentiments that a prosthetics student with a transtibial amputation expressed during a group discussion in one of my behavioral science courses: “Don’t call me ‘a patient’—I’m not sick.”
Words are used to communicate meaning but can have unintended consequences. Sabolich’s focus was on the perception that other medical professionals and the public have about prosthetists and orthotists. The student’s focus was on the implication that he was not well, and he did not view himself this way. What terms most appropriately describe the relationship a clinician has with the individual to whom he or she provides services? This article explores the various terms used for those with whom we work, and how those labels affect their perception of themselves, our attitudes towards them, and the clinical relationship.
Words Matter
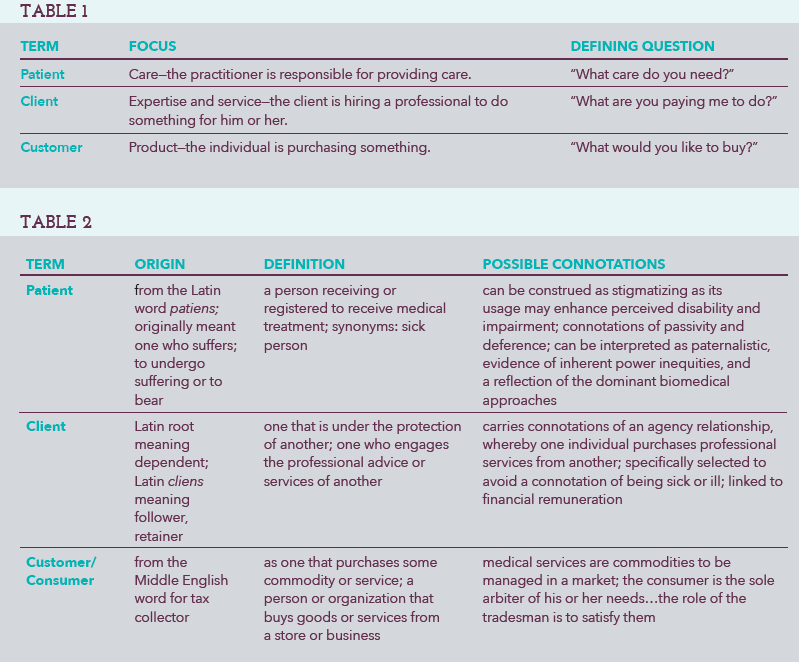
The words we use are informed by and can impact our view of reality and our expectations. Words used to describe a group or class of individuals can define the relationships we have with them and the expectations we bring to those relationships.2 When communicating, the “idea or feeling that a word invokes,” its connotation, can be more important than the “literal or primary meaning.” A recent dinnertime discussion with a group of pre-teens (n = 3) at the Brinkmann household centered around how different labels communicate different things about the levels of care and personal involvement in a relationship. Table 1 contains a summary of this informal consensus process. Table 2 contains the formal definitions of terms commonly used to describe individuals who seek medical care, along with informal connotations of these terms gathered from the referenced articles.
Protecting the right to self-determination and the autonomy of the individual are central tenets of contemporary medical ethics and have been codified into law by mandating that medical providers obtain informed consent from those with whom they work. As medical practitioners have become more aware of these ethical issues and the importance of patient engagement and empowerment, the term patient has come under scrutiny. According to pediatrician Michael Shevell, MD, CM, FRCP, FCHAS, this term implies “passivity (‘object of an action’) that removes responsibility (‘bearing, enduring’)…” and “can be construed as stigmatizing as its usage may enhance perceived disability and impairment. These implications in the construct of ‘patient’ devalue the intrinsic autonomy of the individual to which the label is applied. It is thus best suited for use within a paternalistic model of healthcare relationships focusing on the acute recognition of disease and its management.”2 If the goal of individual empowerment can be undermined by a common term we use to describe those we work with, should we consider exchanging that label for one that affirms that value more explicitly? Shevell suggests that those who use the term client “seek to convey a non-medical, humanistic, less acute care model of orientation to healthcare delivery that is thought to be more empowering to the actual recipient of healthcare.”2
Unfortunately, labels that have been suggested as a replacement for patient, such as client, customer, or consumer, present additional problems, since they can define the relationship primarily as an economic or commercial one. This is problematic in numerous ways. Shevell points out that the origin of the word client relates to “a plebeian who sought the protection and/or patronage of a powerful patrician…The actual root origins of the word hardly convey an aspect of the empowerment quality that was originally sought when employed in healthcare terminology.”2 Most clinicians would agree that medical decision making with a primary focus on the financial implications of decisions often results in suboptimal care.
As Magnezi et al. point out, “A business model for the doctor-patient relationship does not do justice to its complexity. The relentless drive to provide more care in less time is inconsistent with the need to develop a real, complex, intimate, caregiving relationship between doctor and patient.”3 Even more importantly, medical professionals have a responsibility to disclose potential risks and benefits of treatment options, make specific recommendations, and even withhold providing services they believe to be detrimental. These responsibilities are not shared in the same way by businesses selling products to customers. As Wing puts it: “Paternalism is appropriate in certain situations: in families and in professional medical relationships. We no more expect a person with multiple trauma injuries to make management decisions than we expect our infant children to fend for themselves.”4
Their Preference Matters
If affirmation of individual autonomy and self-determination is central to medical ethics, the preferences of individuals seeking medical care must be considered. According to Magnezi et al., “…when one actually asks patients who are receiving medical treatment…how they would like to be addressed, most respond, patient.”3 In 1997, Wing, a Canadian orthopedist, surveyed “a group of people attending an ambulatory back-pain clinic in a teaching hospital,” and 101 individuals were given a short letter and survey asking them to indicate whether they preferred the term client or patient.4 “Almost three-quarters (74) stated a preference for patient, and 19 chose client; the remaining eight had no preference.”4
In the same year, Deber et al. surveyed individuals receiving care in two different settings.5 One group (n = 611) was receiving treatment for breast cancer, prostate cancer, fractures, spina bifida, and low back pain in “three outpatient clinics in an urban teaching hospital.”5 The other group comprised individuals (n = 431) living with HIV/AIDS who were enrolled in a national database. Participants ranked their preference for the terms “patient, consumer, customer, client, partner, and survivor” on a five-point Likert scale from strongly dislike to strongly like, and completed scales measuring decision making and trust in the physician. “All populations moderately liked the label ‘patient’…. No other label went beyond the indifference range, and most terms evoked negative scores…with particular rejection of the terms ‘customer’ and ‘consumer.’ The highest approval for any label other than ‘patient’ came from the HIV population, where the neutral score (0.03) included about one-third liking the term ‘client’; although the other clinical populations were less likely to endorse this term.”5 In 2015, Magnezi et al. published research on individual preferences related to the terms “patient, friend, partner, client, consumer, or insured,” the relationship participants had with their physician, confidence in the care provided, and their participation in healthcare. “Participants in the study chose the terms patient and friend over business-type terms, because a business model is inadequate.”3
Relationships Matter More Than Words
If the point of changing labels is to empower individuals and encourage engagement in their own care, it is important to consider whether a change in terminology has the desired effect. When arguing for continued use of the word patient, Debra Jackson, PhD, RN, states, “What has not been evident thus far in the debate is whether changing the designated labels for care-recipients actually transforms the relationship in a positive way.”6 Peters and Cunningham report that “there is little evidence to suggest that people seeking health services who are identified as ‘clients,’ ‘consumers,’ ‘customers,’ and ‘service users’ are any more empowered than those identified as ‘patients.'”7 Research by Magnezi et al. that was designed to identify not only individual label preferences but also to relate label preferences to participation and physician trust levels, found that “…a business-type relationship did not further patient autonomy or participation in care…. Individuals who have the type of relationship they want (no matter what they call it) have greater confidence in the treatment received from their doctor, whereas those with a business-type relationship were less likely to report high confidence in their care.”3 According to Dickens, “more heat than light has been generated about the issue of terminology, but there is no evidence that the issue holds any importance whatsoever for ‘patients,’ or that use of any particular terminology has consequences, positive or negative, for them…most ‘patients,’ although prepared to offer a preference, just did not think it was a terribly important question.”7 To complicate matters, individuals may have different preferences depending on whether they are receiving acute or follow-up care. The prosthetic student mentioned earlier, for instance, considered himself a patient while in the hospital immediately following a traumatic amputation, but did not consider himself one when receiving long-term prosthetic care. If individuals express a preference for some term other than patient, we should use it. The research is clear that if a preference is not expressed, a label change is unnecessary, since the term patient would most likely match the individual’s preference if he or she were asked. Wing suggests that we treat patients “as equals in all but information,” and that concerns about paternalism and autonomy “should be addressed by our continually and critically reviewing how we care for people, with due regard for their ability to make and articulate decisions at different stages of disease, rather than by changing our terminology with no concern for preferences.”4 Shevell’s appeal to common sense and social norms is on target: “When we encounter someone socially, we inevitably ascertain early in our encounter what he or she wishes to be called and through usage, affirm their choice. Thus, the decent and polite thing to do is the one which best promotes self-determination.”2
Conclusion
Shevell’s suggestion that any label used to distinguish between individuals providing and receiving care results in “questioning or diminishing an equality between provider and recipient of moral agency and authority,” and that we should refer to those we work with simply using nouns such as persons, individuals, men, women, or children seems extreme.2 None of those general terms describe the special relationship that we enter into and the responsibility we accept when providing medical care. Magnezi et al. point out that “patients view the doctor-patient relationship as unique. The same patients who desire autonomy also want a caring, human relationship with their physician.”3
In reviewing the literature, Wing identified concerns that “terminology should be situation-specific: ‘patient’ for the acute care situation and ‘client’ for other situations, such as when preventive or palliative care is needed or when a person functioning normally in the community requires a service such as the provision of an orthosis.”4 In other words, he does not consider individuals receiving an orthosis to be patients, perhaps because he understands orthotic management more as the provision of a device or professional service rather than medical care. It appears that the concerns expressed by Sabolich in his 1981 article remain relevant today. How we are perceived by the public, our referral sources, and those we work directly with will be affected by many different factors. Many of these, including our vocabulary, are within our control. It is worthwhile to give thought to how our words and actions can most accurately demonstrate the education and expertise required to provide O&P care.
John T. Brinkmann, MA, CPO/L, FAAOP(D), is an assistant professor at Northwestern University Prosthetics-Orthotics Center. He has more than 20 years of experience treating a wide variety of patients.
References
-
Clinical Prosthetics & Orthotics. 1982. 6(1):10 http://www.oandplibrary.org/cpo/1982_01_010.asp?searchquery=professionalism%20or%20what
-
Shevell, M. I. 2009. What do we call ‘them’?: The ‘patient’ versus ‘client’ dichotomy. Developmental Medicine & Child Neurology 51(10):770-2.
-
Magnezi, R., L. C. Bergman, and S. Urowitz. 2015. Would your patient prefer to be considered your friend? Patient preferences in physician relationships. Health Education & Behavior 42(2):210-9.
-
Wing, P. C. 1997. Patient or client? If in doubt, ask. CMAJ: Canadian Medical Association Journal 157(3):287.
-
Deber, R. B., N. Kraetschmer, S. Urowitz, and N. Sharpe. 2005. Patient, consumer, client, or customer: What do people want to be called? Health Expectations 8(4):345-51.
-
Jackson, D., M. Hutchinson, and S. Wilson. 2016. In defence of patients. Journal of clinical nursing. 25(9-10):1177-8.
-
Peters, K., C. Cunningham, and G. Dickens. 2016. Response to Jackson, Hutchinson & Wilson (2016) Editorial: In defence of patients. Journal of Clinical Nursing. 25(15-16).
Support authors and subscribe to content
This is premium stuff. Subscribe to read the entire article.





