Introduction
Craniofacial prosthetics has been an orphan service for decades—publicized for dramatic effect at one moment and then forgotten the next. Some dedicated anaplastologists are passionate about their vocation, but their numbers are shrinking. The O&P profession holds enormous potential to elevate the levels of sophistication in the design and delivery of craniofacial prosthetic devices. O&P possesses a vibrant, expanding academic and professional infrastructure that would be beneficial to craniofacial prosthetics as a specialty. Craniofacial prosthetics could flourish as a small but serious society within the O&P profession.
Craniofacial Prosthetics
Craniofacial prosthetics is the fabrication and fitting of orbital, nasal, and auricular prostheses using several methods of attachment including adhesives, mechanical means (eyeglasses and dental obturators, for example), anatomical fit, and osseointegration (OI). Craniofacial OI fixtures placed in the mastoid, maxilla, or orbital rim retain the prosthesis via percutaneous abutments and magnetic or clip components. OI science, pioneered by Per-Ingvar Brånemark, MD, PhD, in the early 1980s, first gained international acceptance in dentistry. In 1995, the Food and Drug Administration (FDA) approved extraoral/craniofacial applications, which was followed by insertion of fixtures into the long bones for limb prostheses.
Designing and attaching facial prostheses anchored to the maxilla, frontal, or temporal bone sounds like a discipline delivered only by those with clinician-level training. However, there are no legal restraints in making and delivering facial prosthetics. Anyone with enough basic lab molding skills and initiative can locate prosthesis vendors (Factor II, Lakeside, Arizona, for example), order materials, take facial impressions, mold, tint, and deliver the prosthesis in any setting. Since the late 1970s, facial prostheses have developed a core following of individuals, many of whom already had careers as a materials scientists, dental technicians, medical artists, sculptors, or movie special effects artists—just to name a few. This diverse group came to adopt the professional moniker anaplastologist, and over the last several decades, a core group of 100–150 individuals worldwide has developed the profession of anaplastology. Craniofacial prostheses, somatic prostheses (silicone fingers, toes, etc.), breast prostheses, and ocular (eye) prostheses all fall within the scope of anaplastology. A small group of anaplastologists was interested in establishing a professional credential, which resulted in the formation of the Board for Certification in Clinical Anaplastology (BCCA) in 2002. The first group of clinical anaplastologists was certified in 2008. Anaplastology has enjoyed a loyal core group, but as a movement, it has been stagnant, with international membership fluctuating or shrinking slightly.
Modern Trends in the Provision of Craniofacial Prosthetics
For the decades following World War II, one accepted convention held that extraoral (facial) prostheses were provided by or under the oversight of specialty dentists, referred to as maxillofacial prosthodontists, who received postgraduate fellowships in both intraoral and extraoral prostheses. In practice, though, the few dentists who complete these rare residencies usually do not end up making their own silicone facial prostheses. More often, they limit their time to taking facial impressions and ensuring that the prosthesis (created and fitted by a technician/artist) is satisfactory. Sustaining a dental practice demands intraoral focus, fitting dental appliances, monitoring cancer patient’s oral status, lecturing dental students, etc.
Over the years, the number of maxillofacial prosthodontics residencies in the United States has shrunk from about 13 to only seven, two of which are in the military. It seems that the in-house prosthodontist-technician model may have been eroded by the entrepreneurial pursuits of medical artists or others who welcomed the call to make silicone facial prostheses as itinerant practitioners rather than as technicians/employees. A contributing factor might be the inability of dental institutions to afford both an intraoral technician and an extraoral specialist like an anaplastologist. In the mid-1980s, several major institutions with a prosthodontics or ear, nose, and throat (ENT) department created positions for head and neck prosthetists, medical sculptors, facial prosthetists, or anaplastologists. Over the last few decades, however, those positions have been eliminated.
Duke University, the University of Nebraska, University of Iowa, University of Texas Health Science Center at San Antonio, and most recently Texas A&M College of Dentistry are among the institutions that have retired their anaplastologist positions and craniofacial prosthetics services. Notably, Roswell Park Cancer Center in Buffalo, New York, had a maxillofacial technician years ago, but in recent years has instead enlisted remote anaplastology consultants to create facial prostheses. Very recently, their website featured their own staff prosthodontist who creates facial, breast, nipple, and other silicone pieces for patients.
Anaplastologists who are based in dental schools have often been tasked with making and delivering partial hand, foot, and breast prostheses, as well as other silicone appliances. There is no absolute ownership of these prosthetic services, and accepting patients is often decided by economic factors.
Given the inherent limitations involved with the dentist-technician model, an independent approach is a worthy alternative practice model. As a medical artist, opening an office in 1985 tested the viability of operating independent of maxillofacial prosthodontists in private practice or at Baylor College of Dentistry. It was found that surgeons who create auricular, midfacial, and orbital defects in treating cancer were receptive to marketing from outside the conventional medical-dental networks and would increasingly refer their patients to the medical artist with an office dedicated to auricular, nasal, and orbital prostheses. For a few decades, this model has been emulated by a string of graduates of the University of Illinois at Chicago (UIC) Biomedical Visualization program and others who have proven through a very few private practices around the country that craniofacial prostheses could be created and delivered not only safely, but perhaps more effectively, by the entrepreneurial artistic individual who opens and equips a standalone facial prosthetics office expressly for this patient population.
Dentistry has served as an academic steward of extraoral prosthetics, committing the training, clinics, and labs to care for patients in need of craniofacial services; however, independent practitioners have invigorated a quest for heightened clinical methods, consistent delivery, and improved aesthetic outcomes. Membership in the American Academy of Maxillofacial Prosthetics is only open to licensed dentists or to those involved in non-independent or indirect patient care as directed by a dentist.
Access Challenges for Patients
An alternative delivery model now exists for craniofacial prostheses. Creating a craniofacial prosthetics specialty ensures that patients can find a dental/medical center with staff or an independent anaplastologist/ocularist, or other competent person, who is willing to make such a prosthesis when needed. There is a nationwide scarcity of individuals who are ready and willing to make or provide these silicone devices, and the trend is worsening. For a prospective artist without another source of income, the economics of starting a private practice supported primarily by facial prosthetics referrals is next to impossible. Many technicians and artists might have the essential skills, but few have the money and time to start an office and wait for a critical mass of referrals to sustain an office and staff.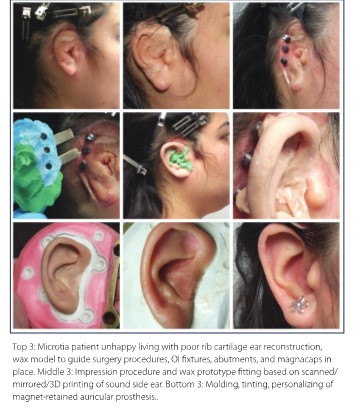
The single training opportunity that helped prepare anaplastologists since the late 1980s (the maxillofacial prosthetics clinic within the UIC Biomedical Visualization master’s degree program) was suspended indefinitely about five years ago. The only civilian domestic introduction to facial anaplastology practice listed on the BCCA website requires a bachelor’s degree, four science courses, and four art courses, but it also relies heavily on submitted art portfolio pieces, and upon completion it provides a certificate of attendance.1 Clearly, more clinical experience is needed beyond this. Ultimately, patients who need facial prostheses are often hundreds of miles from a capable practitioner. Even large cities often lack a prosthetic provider that actively advertises the capability to design and fabricate facial and somatic prostheses. For this reason, my practice is developing creative methods of transferring knowledge to credentialed O&P practitioners who are willing to receive these patients.
At this writing, the BCCA website lists just 37 certified clinical anaplastologists (CCAs) in the United States. Of this group, a number offer other services like breast and somatic prostheses, ocularistry, or medical graphics and photography services to sustain their practices, and some have moved into administrative or teaching activities. Because patients in many parts of the country do not have a clear path to a practitioner with clinical credentials on par with O&P, many craniofacial patients likely forego treatment because they cannot afford or are unwilling to travel out of state, or they find the final prosthetic result disappointing and ineffective for use, and some may be dissuaded by physicians who have formed a poor opinion of facial prosthetics services and outcomes.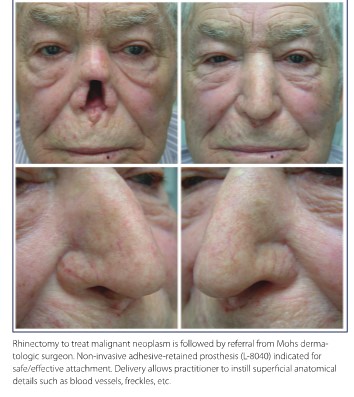
Higher education and clinical training are clearly lacking in craniofacial prosthetics. In the United States, there are no clinical training programs or residencies that focus on craniofacial prosthetics in the way that O&P prepares its graduate students. Anaplastology courses may exist as electives in a few medical illustration curricula, dental technician programs, or other fabrication-based programs. Prosthetics vendors like Factor II and retired anaplastologists have occasionally offered courses in molding silicone prostheses, but none of these opportunities lead to advanced levels of clinical application or imply competency as an allied health professional to treat patients with prostheses. Anaplastology’s engine is fabrication, but without more clear pathways leading to clinical credentials and patients, it stalls. Anaplastology is off the radar of most pre-healthcare students and more often catches the attention of medical illustrators and technicians who have excellent art skills but who will likely lack chemistry, physics, engineering, and clinical training.
What Does Anaplastology Have to Do with O&P?
It is important to understand the different backgrounds of those creating craniofacial prostheses to consider how craniofacial prosthetics might be advanced in a different way and to a greater degree from either the dentistry or the anaplastology realm. Given the scientific and professional framework that exists within the O&P profession, perhaps it is time for a certain number of orthotists or prosthetists to bring craniofacial prosthetics projects into traditional O&P settings.
One might compare craniofacial orthotics to craniofacial prosthetics. Is the purpose of correcting cranial disfigurement so different than correcting facial disfigurement? Like cranial orthotics, there are both aesthetic and functional aspects to craniofacial prostheses. Beyond the restoration of facial aesthetics, the rehabilitative protection of compromised tissue beds, restoration of airways, sound locations, and support of eyeglasses are just a few functions of orbital, nasal, and ear prostheses. The patient population is different, but the sciences of head and neck anatomy, the technologies that can be adopted (like scanning and 3D printing), engineering principles, delivery or devices, follow-up care, publication, and evidence-based practice could all be shared. The richness of O&P scientific societies, meetings, and multiple publications could all contribute to elevating and enhancing the patient experience and the professional satisfaction among practitioners. With the exception of intraoral or invasive prosthetics like implants, O&P clinicians have earned the right to apply their skills to prosthetic device delivery across the entire body.
OI exists in both craniofacial and extremity prosthetics, and the management of abutments and attachments are very similar. Loss of facial form and loss of limb have similar impacts on patients psychosocially, and the technology used to restore animation and movement may overlap across both disciplines. Just as targeted muscle reinnervation has helped to restore sensation in prosthesis users, orbital reanimation has been attempted with facial prosthetics. And there does seem to be recent interest by prosthetists. In “Additive O&P” in the April 2021 issue of O&P Almanac, the prosthetists who were interviewed mentioned that they 3D print nasal and ear prostheses and face masks for orbital and maxillofacial patients. This would indicate some level of interest and competence among prosthetists in receiving and treating craniofacial patients. In the same issue, the article “Accelerating Acceptance” mentions that prosthetists are becoming more integrated into medical teams where they are seen as key authorities in OI and neural implant cases. This would suggest some prosthetists have established a commendable level of respect among physicians and surgeons for their clinical contributions involving percutaneous OI attachments. Therefore, some prosthetists will be receptive to creating craniofacial prostheses that are bone anchored. If a number of these early adopter prosthetists in each state will receive patients, the problem of access may be alleviated.
O&P is an established profession with multiple associations that support its 13 degree programs, residencies, certifications, licensure, and professional and legislative issues, as well as multiple publications for disseminating clinical, technical, and professional information. With these vast resources and practitioners’ confident treatment of patients from head to the toe, it seems odd that there has not been more interest in treating patients in need of craniofacial prostheses.
Creating and Delivering Craniofacial Prostheses
Conventional adhesive-retained facial prostheses are often billed in the $5,000–$10,000 range, with OI versions being billed at twice the amount of non-implant versions. Physicians and dentists sometimes submit claims using CPT codes (for example, 21086 for an auricular prosthesis), while non-physicians use HCPCS L-Codes L-8040–L-8049 for facial prostheses and V-Codes for artificial eye/ocular prostheses and related services (for example, V-2623, ocular prosthesis, custom, plastic).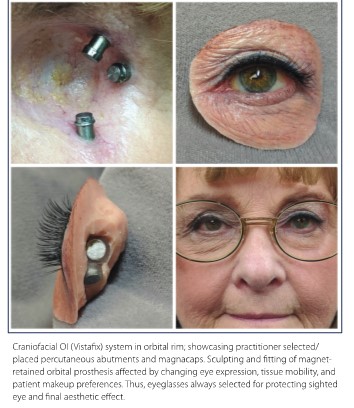
Craniofacial prostheses have been provided in numerous settings. In terms of best practices for the delivery of facial prostheses, each setting has its merits and liabilities, but none should be ruled out since physician awareness of and patient access to any capable practitioner is such a challenge. The author has been involved with delivering craniofacial prostheses in the following models:
- Large medical and dental institution clinics where patients may have received initial treatment for cancer, trauma, or other condition. Here, prostheses may be fabricated and delivered by an artist/anaplastologist/technician with the services being overseen by dentists or physicians.
- An accredited facility for anaplastologists/prosthetists specializing in the design, fabrication, and fitting of craniofacial and other prosthetic categories.
- Dental offices where a medical artist develops and delivers the prosthesis but uses a small oven and tools at home for mold fabrication and processing.
- An ocularist’s office where the ocularist may make and fit facial prostheses along with artificial eyes or allows an anaplastologist to use part of the office to fabricate, fit, and bill for facial prostheses separately.
- A professional/executive day office where the practitioner captures much of the needed patient information, then delivers the finished prosthesis a day or two later in person or by mail.
To safeguard patients, Medicare imposes limits on the creation and delivery of prostheses, yet it is permissible for providers to send finished facial prostheses through the mail to the patient with the mail receipt retained in the chart as adequate proof of delivery.
In the absence of established prosthetics clinics, our practice and others may accept inquiries from patients and teams with physicians beyond state borders who are willing to collaborate at a distance to provide needed craniofacial prostheses. ENT and plastic surgeons from across the United States are often receptive to collaborating with prosthetics practitioners in learning the Vistafix OI system (Cochlear Americas, Centennial, Colorado) to place fixtures to support craniofacial prostheses. Distance care is more challenging on all levels, but with experience and the trajectory of technology, any safe provision of quality prosthetic results is better than a total lack of access.
O&P practitioners, especially those with a facility, have an advantage to expand their scope of practice. Many have established worldwide visibility on the internet and gained a fulfilling sense of autonomy and identity as authorities in OI care, as referenced earlier. This has positioned these practitioners to receive physician- and self-referrals directly, thus empowering them to facilitate pre-prosthetic surgical planning with referring physicians or referral of patients to new physicians, further cultivating their network and status. The certified and/or licensed prosthetist has the advantage of communicating with surgeons involving invasive treatments because they possess a widely accepted and respected clinical credential.
The basic process of sculpting a wax nose or ear, investing it in a dental stone mold, and packing and processing a silicone prosthesis is quite simple and could be taught to any O&P practitioner or fabricator in a morning or afternoon. In fact, the sculpting, molding, tinting, and delivery of a conventional auricular or nasal prosthesis is very comparable to the production and delivery of an aesthetic/passive silicone finger prosthesis. The timeline is also similar, consisting of impressions, a sculpting and color-matching session, the fabrication of a two- or three-piece stone mold/silicone, packing/processing, and a final session to tint and deliver the prosthesis with instructions. Facial prostheses do not involve shrinkers or check sockets. Additionally, each type of facial prosthesis has a unique L-Code (for example, L-8040, nasal prosthesis provided by non-physician) that can be pre-authorized and reimbursed in a more predictable way than the not-otherwise-specified code L-7499 that accompanies all upper-extremity passive silicone appliances. All materials used in creating every type of orbital, nasal, and auricular prosthesis, including OI components (magnets, abutments, etc.), are available from several vendors. As with any O&P skill, the ability to refine techniques with each new case and fashion a slightly more novel design with each successive patient can be very satisfying. An example of this technique refinement would be the design of a hollow, lightweight orbital prosthesis or a magnet-retained nasal prosthesis, both of which are more complex to fabricate but eliminate the need for adhesives. In cases like these, watching patients easily position their prostheses and smile at delivery can be immensely rewarding. Scanning and 3D-printing technology have helped to increase the accuracy of craniofacial prosthetics. It is exciting to imagine how other materials and technologies that are used in O&P might be applied to craniofacial prosthetics.
Summary
Craniofacial prosthetics has been treated as a sideline service provided by anaplastologists, dentists, ocularists, and perhaps prosthetists. In the United States, many medical and dental institutions that once touted craniofacial prosthetics have eliminated these services and related staff. There are a handful of anaplastologists committed full time to the specialty, but the anaplastology field and its service to patients is limited by small membership numbers, a lack of training programs, and the economic challenges related to sustaining a business that is dependent on craniofacial prosthetic referrals. The prostheses provided by anaplastologists and others may be artfully created, but access to skilled practitioners continues to be a challenge for patients. This is evidenced by hundreds of inquiries a single specialty website will receive from prospective patients across the country, including many from densely populated medium and large cities. Furthermore, the provision of the devices by a loose network of diversely educated low-profile individuals has a diluting and isolating effect on this important service. No profession currently claims definitive authority over or ownership of craniofacial prosthetics as a specialized discipline. These important devices could be supported as a professional service, perhaps more effectively, by the principles and practices of the O&P profession. Orthotists and prosthetists with interest should consider receiving patients in their area who need a craniofacial prosthesis.
References
- https://medicalart.johnshopkins.edu/anaplastology-training-program/
Further Reading
- “Fundamentals of Facial Prosthetics,” by Robert E. McKinstry 1995, Abi Professional Publications; 224 pages.
- Is O&P a Profession? Jason Highsmith (article in AAOP Journal a few years ago)
- Blinking Orbital Prosthesis Model Based on Biomechanical Principles: The Embedded Tension Mechanism (ETM) Michael J. Konrath, Blake J. Marzella, Justin T. Cacciatore, Bret M. Olson, Jeff R. Groskopf, Michael T. Musser, Gregory G. Gion, M.M.S.
- Volume 5 – number 1 – International Journal of Anaplastology – November 2011
Accelerating Acceptance; April O&P Almanac ISSN: 0968-7599 (Print) 1360-0508 (Online) Journal homepage:
https://www.tandfonline.com/loi/cdso20
Links
- https://www.bcca-cca.com/certified-clinical-anaplastologists
- https://medicalart.johnshopkins.edu/anaplastology-training-program/
- https://www.maxillofacialprosthetics.org/students/student_programs
- https://www.roswellpark.org/cancertalk/202105/restoring-appearance-through-art-science-prosthetics
Video
- https://www.youtube.com/watch?v=rmm47xLRw-E.






